By Claire Cowley
Experts have warned City leaders about alarming numbers of opioid-related deaths among African-Americans on Chicago’s South and West Sides during the coronavirus (COVID-19) pandemic.
Natalia Derevyanny, director of communications for the Cook County Bureau of Administration, said, “I am noticing a spotlight starting to shine on all the other challenges our communities are facing” during the pandemic, one of those being the opioid crisis.
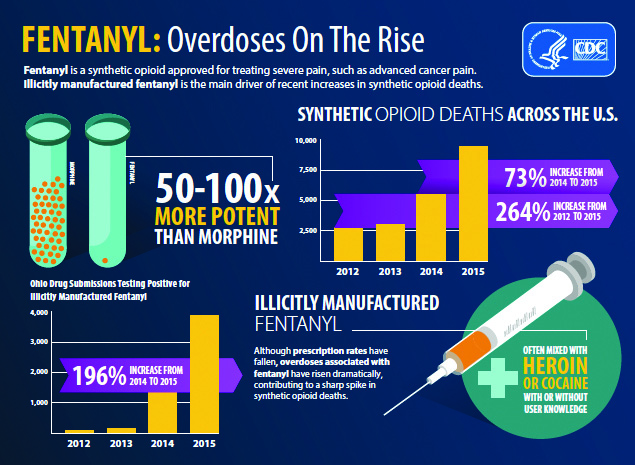
Overdoses of the opioid fentanyl are on the rise, according to the Centers for Disease Control.
Derevyanny said the Cook County medical examiner’s office started to notice the uptick of opioid-related overdoses right around the time they started getting COVID-19 cases.
“Both of these issues are disproportionately affecting our traditionally underserved communities, most often our African-American” communities, Derevyanny said.
“This has been a particularly difficult year for so many reasons,” she added. “We usually have 6,000 to 6,500 overdose cases a year. This year we’re already over 9,400 overdose cases.”
Derevyanny said the Black population comprises about 50% of opioid overdose cases, although Blacks make up only about 23% of the Cook County population.
“It’s double where it should be,” Derevyanny said, although the number “should be zero.”
Derevyanny said that, in an ideal world, a given health challenge would affect the population proportionately across demographics (such as race) based on the percentage each demographic represents within the total population. Yet a drastic number of African-Americans are suffering.
Lethal cocktail
According to the Cook County medical examiner’s case database, statistics show a prevalence of mostly middle-aged Black males using a lethal cocktail of drugs and opioids.
The database shows most overdose victims combine cocaine and heroin with prescription drugs such as tramadol and two types of fentanyl.
Derevyanny said her administration is looking for these specific opioids, including synthetic fentanyl, so officials can alert police or public health departments.
“I think knowledge is power,” she noted. “We’re always looking for patterns, and the more eyes we have on the challenges, the more people are involved in finding solutions.”
Ngozi Ezike, MD, director of the Illinois Department of Public Health, said that, in early 2020, Governor JB Pritzker signed the Overdose Prevention and Harm Reduction Act to establish and operate a needle and hypodermic syringe access program.
Ezike added the life-saving drug naloxone and access to medication-assisted therapy can help. “Access to safer drug use and harm reduction supplies reduces the transmission of infectious diseases and prevents overdoses,” she said.
IDPH is working with the Illinois Department of Human Services Division of Substance Use Prevention and Recovery and the Helpline for Opioids and Other Substances on a harm reduction and media campaign to connect individuals and their loved ones to services.
“We want them to know they are not alone,” Ezike said.
Lack of access to behavioral health services, including mental health and substance use treatment services, plays a major role in this epidemic, she explained.

The numbers show opioid use is an epidemic, according to the U.S. Department of Health and Human Services.
Treatment harder to access
Thomas Britton, president and CEO of the Gateway Foundation, said treatment is harder to access during the pandemic, resulting in a drug use and relapse rate increase.
Also, the nature of any substance abuse disorder makes it a disease of social isolation.
“What we have seen from the stay-at-home orders is the fear of losing one’s job, economic challenges, boredom, and loneliness bringing up a lot of emotion most people typically use drugs as an antidote for,” Britton said.
The more people are by themselves and left to their own devices, the harder it is to not use drugs and stay in recovery.
“And then the compound factor is the drugs available on the streets are higher in fentanyl than normal because heroin has been harder to get,” Britton said. Put these two together, and people are taking a much more lethal drug.
Alicia McGhee, information coordinator for the Chicago Department of Public Health, said the City is increasing options available to provide telehealth services, so people can obtain drugs used to treat opioid use disorder safely.
On the state level, McGhee said the governor mandated in an executive order that all insurance companies regulated by the Illinois Department of Insurance cover the cost of telehealth services.
She added the City is working to address systemic health inequities by taking immediate steps to minimize gaps in healthcare systems and creating more equity in programs to help vulnerable populations.
“Through a partnership with West Side United, the City’s racial equity rapid response teams have been working to reach the vulnerable population most impacted by COVID-19,” McGhee said.
Guided by the data, the City has developed a hyper-focused strategy centered around deep, consistent education, outreach, and intervention, McGhee explained.
Antonio Jimenez, director of the Community Outreach Intervention Project, said people have come to them during the pandemic.
“That’s why we saw ourselves as essential to keep people alive and prevent them from overdosing,” Jimenez said.
Jimenez said the most successful program reaching people has been the project’s syringe exchange program.
This program is driven by the need for people to access injection drug-use supplies at COIP field sites where opioid users can exchange their used syringes for clean ones, Jimenez added.
“Most of the work was done at our doorways at our field stations…right in front,” Jimenez said. “We were able to maintain basic services for people who can’t come in the office unless they have a clinical or case management need.”
Jimenez said four in five communities around the city are marginalized and impacted by poverty, racism, inequality or lack of services.
“We provide a vital service…although our work focuses on substance using populations, we do get community members who aren’t substance users coming in to use or seek help,” Jimenez said.
The COIP is funded by a variety of sources such as the Illinois Department of Health, State of Illinois Substance Use Prevention and Recovery Division, and Illinois Department of Public Health, Jimenez added.
“COVID impacted us greatly…like a lot of other organizations,” Jimenez said.
Jimenez said it is hard for organizations in this new environment to work virtually or remotely because community members prefer in-person discussions to talk about issues.
“Our staff who are not technologically proficient have experienced a learning curve on how to use equipment to stay in touch with clients,” Jimenez said, adding that COIP’s goals are to reach more people and make their lives as healthy as possible.
For the Chicago Department of Public Health, call (312) 747-9191, email McGhee at [email protected], or log on to www.chicago.gov/city/en/depts/cdph.html. For the Cook County Bureau of Administration, call or email Derevyanny at (312) 603-8286 or [email protected], or log on to www.cookcountyil.gov/agency/bureau-administration-0. For the Cook County Department of Public Health, log on to https://cookcountypublichealth.org/. For the Gateway Foundation, call (312) 316-1412 or log on to www.gatewayfoundation.org/. For the Community Outreach Intervention Project, call (312) 996-5523, email Antonio Jimenez at [email protected], or log on to https://coip.uic.edu/. For Substance Abuse and Mental Health Services Administration, log on to https://www.samhsa.gov/newsroom/press-announcements/202008270530, call 240-276-2130 (press 4).
